The Centers for Advanced Orthopaedics is redefining the way musculoskeletal care is delivered across the region with locations throughout Maryland, DC, Virginia and Pennsylvania.
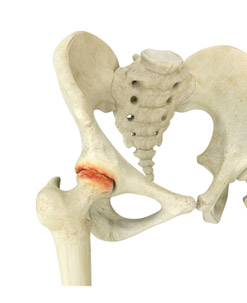 Osteoarthritis of the hip, also called degenerative joint disease, is the most common form of arthritis. It occurs most often in older people, however, it can occur in younger patients with previous hip conditions including femoroacetabular impingement, hip dysplasia, trauma, avascular necrosis, slipped capital femoral epiphyses, and legg-calves-perthes disease. In a person with osteoarthritis, the cartilage becomes damaged and worn out creating bone-on-bone contact in the joint. This causes pain, swelling, stiffness, and restricted movement of the affected joint. Osteoarthritis may affect various joints in the body including the hips, knees, hands, and spine, the hip joint is the most commonly affected.
Osteoarthritis of the hip, also called degenerative joint disease, is the most common form of arthritis. It occurs most often in older people, however, it can occur in younger patients with previous hip conditions including femoroacetabular impingement, hip dysplasia, trauma, avascular necrosis, slipped capital femoral epiphyses, and legg-calves-perthes disease. In a person with osteoarthritis, the cartilage becomes damaged and worn out creating bone-on-bone contact in the joint. This causes pain, swelling, stiffness, and restricted movement of the affected joint. Osteoarthritis may affect various joints in the body including the hips, knees, hands, and spine, the hip joint is the most commonly affected.
Diagnosis
The diagnosis of osteoarthritis of the hip is made by a detailed medical history and physical examination. X-rays are helpful in showing decrease in joint space, consistent with articular cartilage loss. MRI scans may show bone bruising and loss of cartilage, consistent with osteoarthritis.
Treatment
Conservative treatment is usually the first-line treatment:
- Activity modification
- Physical therapy
- Non-steroidal Anti-Inflammatory Drugs (NSAIDs)
- Topical medications such as ointments can be applied over the skin
- Weight loss
- Intra-articular cortisone and viscosupplementaion injections can provide pain relief.
In cases of severe osteoarthritis or when conservative treatments fail, surgical intervention (Total Hip Replacement/Arthroplasty) is the considered. A total hip replacement involves removing existing arthritis and placing a metal cup in the socket (acetabulum) and a metal stem into the hollow of the thigh bone (femur). Usually there is a plastic (polyethylene) liner, sometimes a ceramic liner, that is placed between the metal ball and socket to provide non metal-on-metal weight bearing surfaces.